Vitamins B and C Might Be the Secret Sauce for Better Blood Sugar
Why Insulin Resistance and Vitamin Deficiency Are More Connected Than You Think
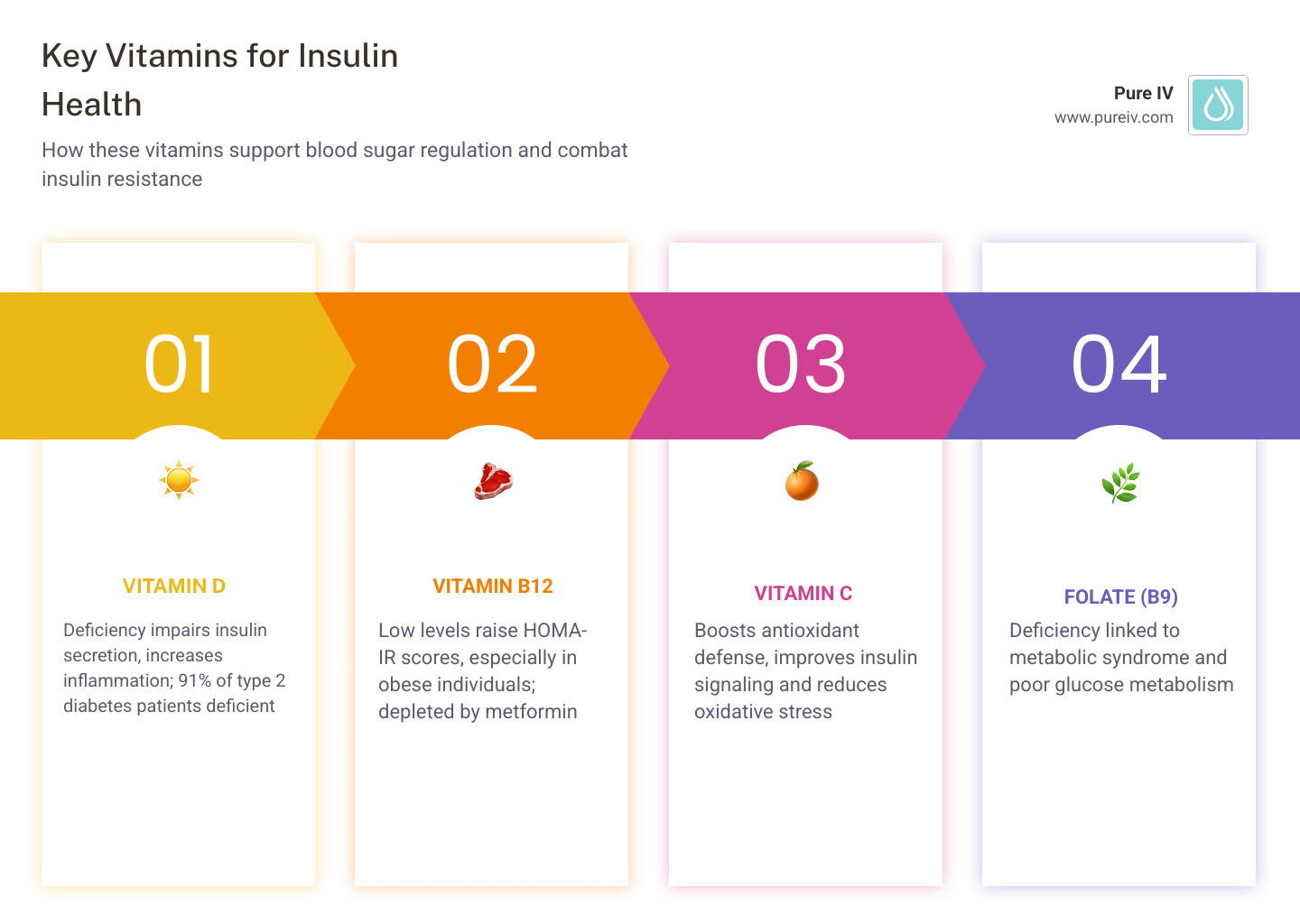
Insulin resistance and vitamin deficiency are closely linked — and fixing one may help with the other. Here's a quick snapshot of what the research shows:
| Vitamin | Link to Insulin Resistance |
|---|---|
| Vitamin D | Deficiency impairs insulin secretion and increases inflammation; 91% of type 2 diabetes patients are deficient |
| Vitamin B12 | Low levels correlate with higher HOMA-IR scores, especially in obese individuals |
| Vitamin C | Supports antioxidant defense and may improve insulin signaling |
| Folate (B9) | Deficiency associated with metabolic syndrome and impaired glucose metabolism |
The numbers are striking. In western countries, up to half of all adults have mild to moderate vitamin D deficiency. And among people with type 2 diabetes, that figure jumps to 91%. Meanwhile, global diabetes cases are projected to climb from 382 million to 592 million by 2035.
That's not a coincidence.
Scientists are increasingly finding that low levels of key vitamins don't just accompany metabolic problems — they may actively make them worse. At the same time, conditions like obesity and insulin resistance can deplete vitamin levels, creating a feedback loop that's hard to break without addressing both sides.
This guide breaks down exactly how vitamins B and C (and their partner, vitamin D) affect your blood sugar, what the clinical evidence actually says, and what you can do about it.
I'm Dr. Allison Lane, a board-certified emergency medicine physician and fellowship-trained sports medicine specialist with over 15 years of clinical experience — including my current role as Medical Director at Pure IV, where I oversee evidence-based nutrient therapy protocols directly relevant to insulin resistance and vitamin deficiency. The research in this area has real implications for how we support metabolic health, and I'll walk you through what you need to know.
The Hidden Link Between Insulin Resistance and Vitamin Deficiency
When we think about metabolic health, we usually focus on the "big" things: how many carbs we eat, how many miles we run, and what the scale says. But underneath those metrics, there is a complex microscopic dance happening. Every chemical reaction in your body—including how your cells respond to insulin—requires specific micronutrients to act as cofactors.
Epidemiological studies have pulled back the curtain on a massive global issue. We are seeing a worldwide explosion in metabolic disorders. According to Global estimates of diabetes prevalence , the number of people living with diabetes is expected to hit nearly 600 million in the next decade.
At the same time, we are seeing a "silent" epidemic of micronutrient depletion. Even in sunny states where we operate, like Arizona, Nevada, and New Mexico, vitamin D deficiency is rampant. In fact, scientific research on Vitamin D and insulin resistance shows that vitamin D deficiency is detectable in 91% of patients with type 2 diabetes. Severe deficiency affects about 32% of those patients.
Why is this happening? The modern "Western diet" is often high in calories but low in micronutrient density. We are essentially overfed but undernourished. This creates a state of insulin resistance and vitamin deficiency that feeds into metabolic syndrome—a cluster of conditions including high blood pressure, high blood sugar, and excess body fat around the waist.
Interestingly, the link isn't just one-way. While low vitamin levels can impair your metabolism, having insulin resistance can also lower your vitamin levels. For example, individuals with higher serum concentrations of vitamin D have a 51% reduction in the risk of developing metabolic syndrome. Conversely, each 10 nmol/L increase in vitamin D levels is associated with a 4% lower risk of type 2 diabetes.
How Vitamin D Deficiency and Insulin Resistance Impact Beta-Cell Function
To understand why vitamins matter for blood sugar, we have to look at the pancreas. Specifically, we need to look at the pancreatic islets, where beta cells live. These cells are the "insulin factories" of your body.
For a beta cell to release insulin, it needs to sense glucose and then trigger a series of internal signals. Calcium is the primary trigger for this release. This is where vitamin D comes in. Research on Vitamin D and pancreatic secretion has shown that vitamin D receptors (VDR) and calcium-binding proteins, such as Calbindin D28k, are present directly within these pancreatic cells.
When you have a vitamin D deficiency:
- Calcium signaling fails: Without enough vitamin D, the beta cells can't manage calcium properly, leading to "sluggish" insulin release.
- Beta-cell exhaustion: The cells have to work harder to produce less insulin, eventually leading to dysfunction.
- Increased apoptosis: Low vitamin D levels are linked to higher rates of beta-cell death, which is a hallmark of the progression from insulin resistance to full-blown type 2 diabetes.
In animal models, vitamin D3 has been shown to rapidly normalize insulin secretion and glucose tolerance. In humans, the presence of these receptors suggests that vitamin D isn't just for "bone health"—it's a fundamental part of the endocrine system that manages your blood sugar.
Addressing Insulin Resistance and Vitamin Deficiency Through Targeted Supplementation
If deficiency causes problems, can supplementation fix them? The answer is a nuanced "yes," especially if you catch the problem early.
For individuals with prediabetes, the stakes are high. A meta-analysis of Vitamin D for prediabetes found that vitamin D supplementation significantly reduced the risk of progressing to type 2 diabetes. Specifically, individuals in the highest quartile of serum vitamin D had an 82% lower risk of developing the disease compared to those in the lowest quartile.
However, the "secret sauce" isn't just taking any supplement; it's about achieving therapeutic dosing. Many over-the-counter vitamins aren't absorbed well, especially in people with high BMI. Fat tissue can actually "sequester" vitamin D, pulling it out of the bloodstream and making it unavailable for your cells to use. This is why we often see better results with high-dose protocols or IV delivery, which bypasses the digestive system's absorption hurdles.
The Science of Sunlight: How Vitamin D Regulates Blood Sugar
Beyond the pancreas, vitamin D acts as a powerful systemic regulator. It behaves more like a hormone than a vitamin, modulating over 200 genes—about 3% of the entire human genome.
In a comprehensive Review of Vitamin D and Type 2 Diabetes , researchers highlighted several biological mechanisms:
- Systemic Inflammation: Vitamin D reduces the production of pro-inflammatory cytokines like TNF-alpha and NF-κB. This is crucial because chronic, low-grade inflammation is a primary driver of insulin resistance.
- SIRT1 Activation: Vitamin D helps activate SIRT1, a "longevity protein" that improves how your cells use energy.
- Irisin and Adiponectin: These hormones help regulate glucose and fatty acid breakdown. Vitamin D levels are positively correlated with these "good" metabolic markers.
Cardiovascular Homeostasis
We can't talk about insulin resistance without talking about the heart. Insulin resistance and vitamin deficiency are major risk factors for hypertension (high blood pressure). The research shows that a decrease of just 16 ng/ml in vitamin D levels is associated with a 16% enhanced risk of hypertension. On the flip side, people in the top third of vitamin D levels have a 30% lower probability of developing high blood pressure.
This is because vitamin D helps regulate the renin-angiotensin system, which controls blood pressure and fluid balance. When these systems are out of whack, it creates a "perfect storm" for cardiovascular disease.
Why Vitamins B and C are the "Secret Sauce" for Metabolic Health
While vitamin D gets a lot of the spotlight, vitamins B and C are the unsung heroes of blood sugar management.
The B-Vitamin Powerhouse
- Thiamine (B1): This vitamin is essential for mitochondrial function. Think of your mitochondria as the "engines" of your cells. If you don't have enough B1, your cells can't "burn" glucose efficiently, leading to higher blood sugar levels.
- Vitamin B12: There is a strong negative correlation between B12 levels and HOMA-IR (a standard measure of insulin resistance). Interestingly, many people taking Metformin for diabetes or Semaglutide for weight loss develop B12 deficiencies over time because these medications can interfere with absorption.
- Folate (B9): Low folate is linked to high levels of homocysteine, which can damage blood vessels and worsen the vascular complications of diabetes.
Vitamin C and Oxidative Stress
When your blood sugar is high, your body produces "free radicals"—unstable molecules that cause oxidative stress. This stress damages the insulin receptors on your cells, making them less sensitive to insulin's signal.
Vitamin C is one of the body's most potent antioxidants. A study on Vitamin D and oxidative stress markers suggests that when we combine antioxidant support (like Vitamin C) with metabolic regulators (like Vitamin D), we see a synergistic effect. Vitamin C helps maintain levels of Glutathione (GSH), the body's "master antioxidant," which protects the insulin signaling pathway.
At Pure IV, we often include these nutrients in our IV Packages & Pricing because they work better together. For instance, L-cysteine and Vitamin C can help restore the redox balance in muscle cells, allowing them to take up glucose more effectively.
Clinical Realities: Why Some Trials Fail to Show Benefits
If the link is so clear, why do some randomized controlled trials (RCTs) fail to show that vitamin supplements cure diabetes? This is a point of confusion for many patients in our clinics in Denver, Nashville, and Las Vegas.
According to a systemic review of supplementation effects , there are several reasons for these inconsistent results:
- Baseline Status: If a study includes people who already have "normal" vitamin levels, giving them more won't show a benefit. Supplementation is most effective for those who are actually deficient.
- Obesity Sequestration: As mentioned, fat tissue can trap vitamins. Many trials use a "one-size-fits-all" dose that is too low for someone with a high BMI.
- The "Epiphenomenon" Theory: Some scientists argue that low vitamin D is a consequence of insulin resistance, not the cause. If IR is the root cause, just adding a vitamin without changing diet or activity levels might not be enough to move the needle.
- Measurement Issues: Many studies use surrogate markers like HbA1c instead of the "gold standard" hyperinsulinemic-euglycemic clamp test, which is much more sensitive to subtle changes in insulin function.
The reality is that insulin resistance and vitamin deficiency must be treated as two sides of the same coin. Supplementation works best when combined with lifestyle interventions that improve insulin sensitivity, such as exercise and weight loss.
Frequently Asked Questions about Micronutrients and Blood Sugar
Can Vitamin D supplements reverse my prediabetes?
While "reverse" is a strong word, the evidence is compelling. Meta-analyses show that vitamin D can reduce the risk of progressing from prediabetes to type 2 diabetes by about 15%. When combined with weight loss—perhaps supported by services like our Weight Loss Services —the results are even more significant.
Why do people with diabetes have lower vitamin levels?
It’s a bit of a "chicken or the egg" scenario. High blood sugar increases the excretion of vitamins through the urine. Additionally, the chronic inflammation associated with diabetes "uses up" antioxidant vitamins like C and E. Finally, medications like Metformin can block the absorption of B12.
How much Vitamin D is needed to improve insulin sensitivity?
There is no universal number, but many experts suggest aiming for serum 25(OH)D levels between 80-119 nmol/L. Achieving this often requires higher doses than the standard RDA, especially for those with obesity. We always recommend checking your levels with a provider before starting a high-dose regimen.
Conclusion: A Holistic Approach to Metabolic Health
The connection between insulin resistance and vitamin deficiency is a reminder that our bodies are integrated systems. You can't fix the "engine" (your metabolism) if you don't have the right "oil" (your micronutrients).
Lifestyle interventions remain the cornerstone of health. Regular exercise and a diet rich in whole foods provide the foundation. However, for many of us living in the environments of Salt Lake City, Boise, or Bozeman, maintaining perfect nutrient levels through diet alone is a challenge.
This is where personalized nutrition and mobile healthcare come in. At Pure IV, we provide a bridge. Our mobile IV therapy delivers essential vitamins directly to your bloodstream, ensuring 100% bioavailability. Whether you are looking for an IV Treatment for Fatigue or supporting your metabolic goals alongside medications like Tirzepatide or Retatrutide , we prioritize safety and efficacy.
Every one of our treatments is approved in real-time by a licensed Nurse Practitioner, ensuring that your "secret sauce" for health is backed by medical expertise.
If you're curious about how Ozempic compares to newer options, check out our Cheat Sheet to Mounjaro vs Ozempic or read The Definitive Guide to Best Weight Loss Injection 2026 to see where the future of metabolic health is headed.
Ready to take the next step in your wellness journey? Book Online today and let our licensed nurses bring the clinic to your door.