What Causes Migraines and How to Prevent the Next One
What Causes Migraines — and Why It Matters
What causes migraines is one of the most searched health questions — and for good reason. If you've ever been knocked flat by one, you know it's nothing like a regular headache.
Here's a quick answer:
| Cause Type | Examples |
|---|---|
| Genetic/Neurological | Inherited brain hyperexcitability, ion channel mutations, trigeminal nerve activation |
| Brain Chemistry | Imbalances in CGRP and serotonin, neuroinflammation |
| Hormonal | Estrogen fluctuations, menstrual cycle, perimenopause |
| Environmental Triggers | Stress, poor sleep, bright lights, weather changes |
| Dietary Triggers | Skipped meals, alcohol, MSG, tyramine-rich foods, dehydration |
The short version: migraines are a neurological disease — not just a bad headache. They're driven by a combination of genetics, brain chemistry, and triggers that push your nervous system past its threshold.
Over 1.16 billion people worldwide live with migraines. It's the third most disabling condition affecting the nervous system , yet it's still widely misunderstood — even by the people experiencing it.
This guide breaks down exactly what's happening in your brain during a migraine, what sets attacks off, and what you can do to prevent the next one.
I'm Dr. Allison Lane, board-certified emergency medicine physician and Medical Director at Pure IV, with over 15 years of clinical experience — and understanding what causes migraines is central to how we approach rapid, effective relief for our patients. Let's dig into the science so you can take back control.

Understanding What Causes Migraines: Genetics and the Brain
When we talk about what causes migraines, we have to start with the "hardware." For a long time, doctors thought migraines were just a blood flow problem—vessels in the head dilating and contracting. We now know that's only a small part of the story. Migraine is a complex neurological disorder involving a hypersensitive nervous system.
Research shows that the heritability of migraine is estimated between 34% and 64%. If one of your parents suffers from them, you have about a 50% chance of developing them too. This isn't just bad luck; it’s written in your DNA. Exploring the hereditary nature of migraine has revealed that multiple genes are responsible for how our brain cells (neurons) communicate and how they handle ion transport.
The "Hyperexcitable" Brain
In a "typical" brain, if a light flashes or a door slams, the brain notices it and then moves on. This is called habituation. In a migraine brain, that habituation doesn't happen. The brain stays on high alert, reacting to every stimulus until it reaches a breaking point.
Key brain regions involved include:
- The Brainstem: Acts as the "generator" or starting point of the attack.
- The Thalamus: The brain's relay station that processes sensory information like light and sound.
- The Hypothalamus: Responsible for maintaining internal balance (homeostasis), which explains why changes in sleep or hunger can trigger an attack.
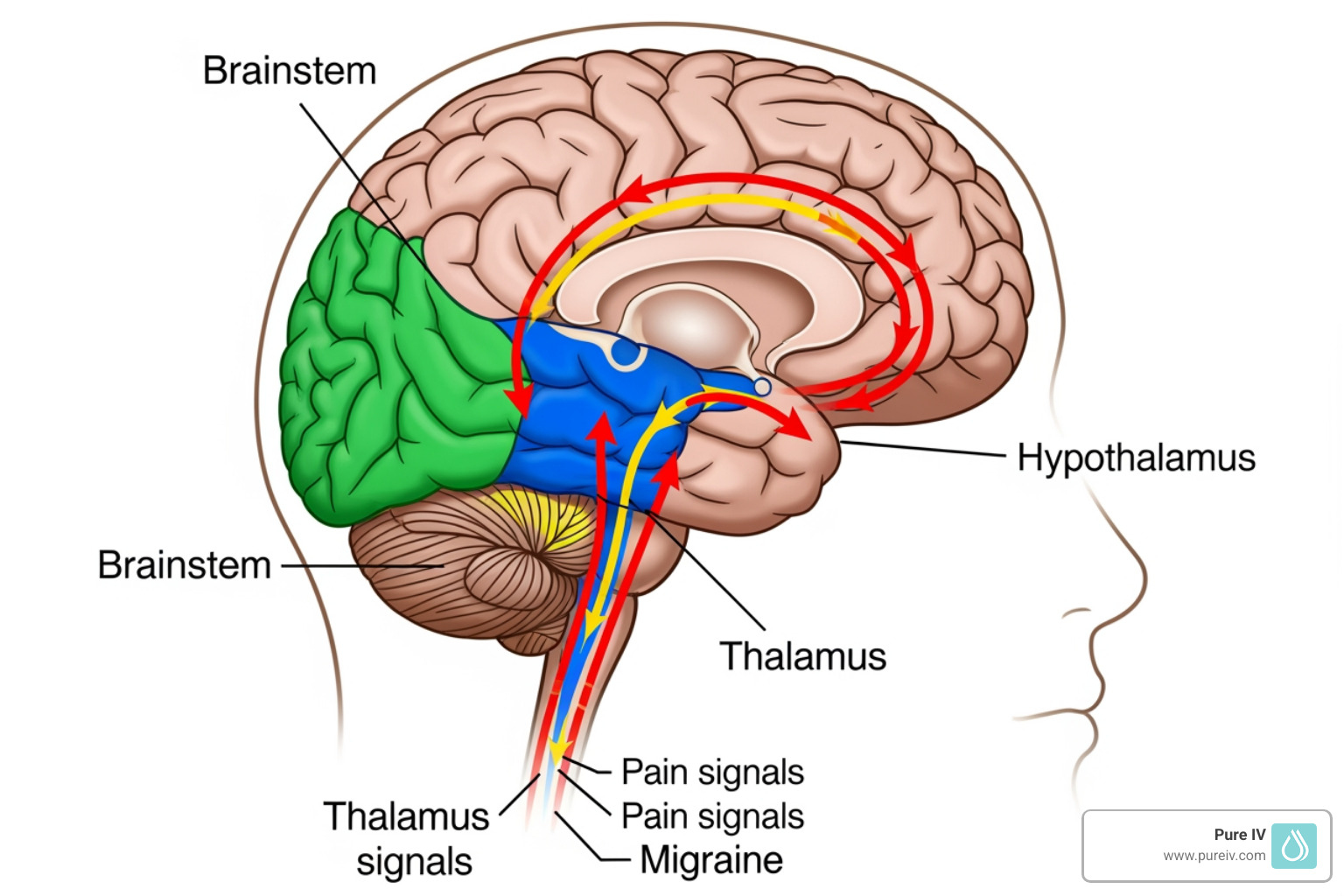
The Role of CGRP and Serotonin in What Causes Migraines
If the brain regions are the hardware, chemicals like serotonin and CGRP are the software. During an attack, the trigeminal nerve—the largest sensory nerve in your head—becomes activated. When this happens, it releases neuropeptides, most notably Calcitonin Gene-Related Peptide (CGRP).
CGRP is essentially a "volume knob" for pain. It causes blood vessels in the meninges (the protective layers of the brain) to dilate and triggers neuroinflammation. This makes the nerves around those vessels extremely sensitive. This discovery has been a game-changer for treatment, leading to the AHS position on CGRP therapies as a first-line preventive option.
Serotonin also plays a major role. Often called the "feel-good" hormone, serotonin helps regulate pain signals in the nervous system. When serotonin levels drop suddenly, it can cause the trigeminal system to release CGRP, starting the painful cascade.
Cortical Spreading Depression and Aura
About 30% of people with migraines experience an "aura." This is usually a visual disturbance—like seeing shimmering lights, zigzag lines (scintillating scotoma), or even losing patches of vision temporarily.
The mechanism behind this is Cortical Spreading Depression (CSD). Imagine a slow-moving electrical wave traveling across the surface of the brain (the cortex) at a rate of about 2 to 3 millimeters per minute. As this wave passes, it first over-excites neurons (causing the "flashing lights") and then leaves them temporarily silenced (causing the "blind spots").
Research on the visual aura neural basis suggests that CSD isn't just a side effect; it may actually be the trigger that activates the trigeminal nerve and leads to the headache phase.
Migraine Triggers vs. Underlying Causes
It is vital to distinguish between the cause and the trigger.
- The Cause: Your genetic predisposition and your brain's "wiring."
- The Trigger: The external or internal event that tips you over the edge.
Think of it like a bucket. Your genetics might fill your bucket halfway. Throughout the day, stress, a skipped lunch, or a thunderstorm add more "water" to the bucket. When the bucket overflows, you get a migraine. This is known as the Threshold Hypothesis.
| Underlying Causes (The Hardware) | External Triggers (The Spark) |
|---|---|
| Genetic mutations (TRESK gene, etc.) | Emotional stress or "let-down" |
| Hypersensitive trigeminal nerve | Weather/Barometric pressure changes |
| Abnormal ion channel function | Strong smells (Osmophobia) |
| Low magnesium levels in the brain | Irregular sleep patterns |
Hormonal Fluctuations and What Causes Migraines in Women
There is a reason women are three times more likely to experience migraines than men. It mostly comes down to estrogen. Specifically, it’s the withdrawal or drop in estrogen that causes trouble.
Many women experience "menstrual migraines" right before or during their period when estrogen levels plummet. This drop affects serotonin levels and increases the brain's sensitivity to pain. Research on estrogen and migraine shows that these fluctuations are often most intense during puberty, pregnancy, and the transition into menopause (perimenopause).
Dietary Factors and Dehydration
While "food triggers" are common, they are also highly individual. What ruins one person's day (like a piece of dark chocolate) might be perfectly fine for another. Common culprits include:
- MSG and Nitrates: Found in processed meats and some savory snacks.
- Tyramine: Found in aged cheeses and fermented foods.
- Alcohol: Especially red wine, which contains tannins and histamines.
Dehydration is one of the most significant—and preventable—triggers we see at Pure IV. When you're dehydrated, your blood volume drops, and your brain can actually shrink slightly away from the skull, pulling on the pain-sensitive membranes. Studies on dehydration and headache confirm that even mild fluid loss can trigger an attack or make an existing one much worse.
Common Environmental and Lifestyle Triggers
Your environment is constantly sending signals to your brain. For someone with a migraine-prone brain, these signals can be overwhelming.
- Stress: Interestingly, many people get a migraine after the stress is over (the "weekend migraine" or stress let-down).
- Sleep: Both too much and too little sleep can be a problem. Consistency is king.
- Sensory Overload: Bright lights (especially blue light from screens), loud noises, and strong perfumes.
- Osmophobia: A hypersensitivity to smells. Research shows that up to 70% of migraineurs experience this during an attack.
- Weather Changes: Shifts in barometric pressure or extreme heat are very common triggers in the states we serve, like Arizona and Nevada.
The Four Phases of a Migraine Attack
A migraine isn't just the time your head hurts. It’s a multi-day event.
- Prodrome (The Warning): Occurs 24–48 hours before the pain. Symptoms include yawning, neck stiffness, food cravings, and mood swings.
- Aura (The Pre-Show): Occurs in 30% of people, lasting 5–60 minutes. Includes visual sparks, tingling in the hands/face, or difficulty finding words.
- Headache Phase (The Main Event): The actual pain, usually throbbing and unilateral (one-sided). Often accompanied by nausea and extreme sensitivity to light/sound.
- Postdrome (The Migraine Hangover): The 24 hours after the pain subsides. You may feel "washed out," confused, or even strangely elated.
How to Prevent the Next Migraine Attack
Prevention is about raising your threshold so those triggers don't overflow your "bucket." We recommend the SEEDS method, a proven framework for lifestyle management:
- S - Sleep: Go to bed and wake up at the same time every day—even on weekends.
- E - Exercise: Regular, moderate aerobic exercise can reduce attack frequency.
- E - Eat: Don't skip meals. Keep your blood sugar stable.
- D - Diary: Track your attacks. This helps you identify patterns you might otherwise miss.
- S - Stress Management: Whether it's meditation, biofeedback, or therapy, managing your cortisol levels is vital.
Non-drug approaches to migraine such as magnesium supplements, riboflavin (B2), and Coenzyme Q10 have also shown significant benefits in clinical studies.
At Pure IV, we focus on that "Optimal Hydration" piece. Because we deliver mobile IV therapy directly to your home or office in cities like Phoenix, Las Vegas, Denver, Nashville, and Salt Lake City, we can help you stay ahead of dehydration-triggered attacks. Our "Migraine Relief" drips often include magnesium and B-complex vitamins, which are scientifically backed to help calm the nervous system.
Frequently Asked Questions about Migraine Causes
Why doesn't my migraine show up on an MRI or CT scan?
This is a source of great frustration for many. An MRI or CT scan looks at the "structure" of the brain—like taking a photo of a computer's hardware. It can show tumors or strokes, but it can't see the "software" (the electrical and chemical signals). Migraine is a functional disorder, not a structural one. We use the IHS classification guidelines to diagnose based on symptoms rather than pictures.
Can stress alone cause a migraine?
In a predisposed person, yes. Stress triggers the release of chemicals like cortisol and adrenaline, which can sensitize the trigeminal nerve. However, for most people, stress is the "final drop" in a bucket that was already getting full from other factors.
Is chronic migraine different from episodic migraine?
Yes. Chronic migraine is defined as having a headache on 15 or more days per month for at least three months, where at least 8 of those days are migraines. This often involves "central sensitization," where the nervous system becomes permanently stuck in a high-alert state. This is different from episodic migraine, where the brain returns to a baseline state between attacks.
Conclusion
Understanding what causes migraines is the first step toward reclaiming your life. It’s not "just a headache"—it’s a biological reality involving your genes, your brain chemistry, and your environment.
While there is no "cure" yet, the combination of lifestyle changes, new CGRP medications, and proper hydration can make a world of difference. At Pure IV, we are proud to be part of your management team. Whether you are in Boise, Albuquerque, El Paso, or Bozeman, our licensed nurses and paramedics provide rapid hydration and nutrient recovery with real-time Nurse Practitioner approval for every single treatment.
If you’re interested in helping move the science forward, we encourage you to look into clinical trials for migraine.
Don't wait for the next attack to start. Stay hydrated, stay consistent, and remember—you don't have to "just push through" the pain. We're here to help.
Pure IV serves multiple locations across Arizona, Utah, Nevada, Colorado, Tennessee, New Mexico, Texas, Idaho, and Montana. All treatments are administered by licensed medical professionals and require NP approval.